Blog
Why Choose Flexible Intramedullary Nails for Bone Fractures?
Bone fractures pose significant challenges in medical treatment. Conventional methods, while effective, may not always provide the best outcomes. This is where Flexible Intramedullary Nails come into play. These devices have gained popularity due to their unique advantages. They adapt well to the natural shape of the bone, offering improved stabilization.
Flexible Intramedullary Nails are noteworthy for their minimally invasive nature. They allow for quicker recovery times and less trauma to surrounding tissues. Physicians note that these nails can lead to favorable healing results. However, not every case may warrant their use. Some fractures may still benefit from rigid fixation methods. This leaves room for discussion on the ideal choice for different fracture types.
In recent years, research has highlighted the increasing success rates associated with Flexible Intramedullary Nails. Yet, there are still concerns and reflections within the medical community. Are there specific scenarios where traditional methods are superior? It's essential to weigh the pros and cons. Ultimately, the goal remains to ensure optimal patient outcomes while embracing innovative solutions.
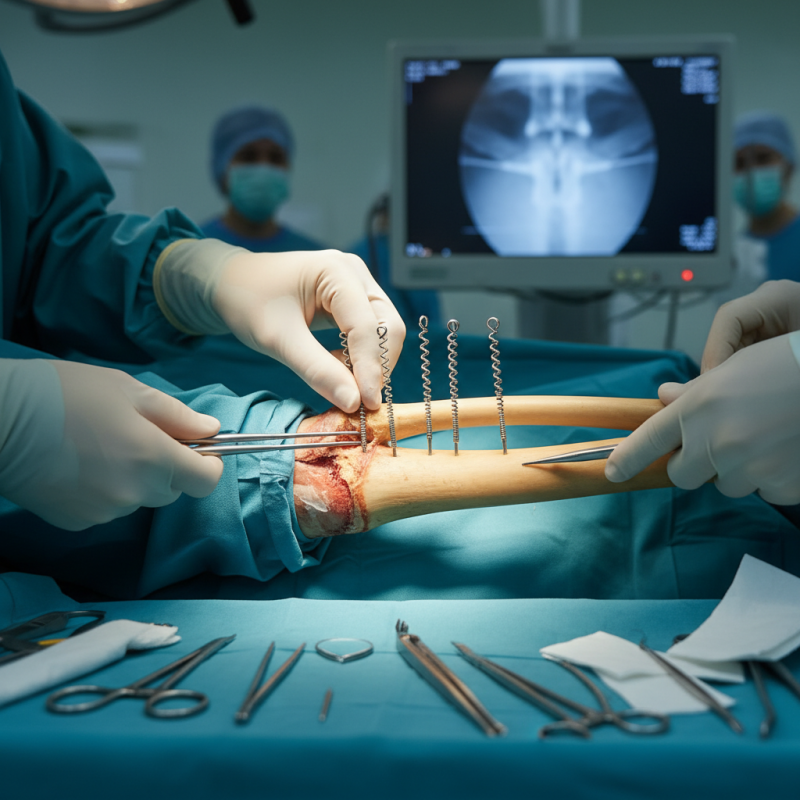
Advantages of Flexible Intramedullary Nails for Bone Fractures
Flexible intramedullary nails are gaining popularity for treating bone fractures. These nails are designed to be adaptable and can fit a range of fracture types. Their unique design allows for easier insertion into the medullary cavity. Surgeons appreciate the flexibility, which reduces the risk of complications.
One significant advantage is the minimized disruption to surrounding tissue. Traditional methods often involve larger incisions. In contrast, flexible nails require smaller openings, leading to less scarring. Patients typically enjoy shorter recovery times and decreased pain levels. However, it's crucial to ensure proper alignment during the procedure. Misalignment can lead to complications, which highlight the importance of skilled practitioners.
The ability to use flexible nails in pediatric cases is also noteworthy. Children's bones are still developing, making these nails an excellent option. They allow for bone growth without hindering healing. Yet, there can be challenges in choosing the right size. Surgeons must assess each case carefully to prevent issues. Overall, flexible intramedullary nails offer many benefits for bone fracture treatment.
Comparison of Intramedullary Nails and Traditional Casting Methods
When considering treatment options for bone fractures, flexible intramedullary nails (IMNs) offer several advantages over traditional casting methods. A study published in the Journal of Orthopaedic Trauma found that IMNs significantly improve healing times for certain types of fractures. Patients using IMNs experienced a 30% reduction in recovery duration compared to those in traditional casts. Faster recovery is crucial for many, especially athletes and active individuals.
IMNs also allow for greater mobility during recovery. Patients can engage in various activities without worrying about compromising the fracture site. In contrast, casts often restrict movement, leading to muscle atrophy over time. Research indicates that up to 25% of patients in casts experience functional limitations post-recovery due to prolonged immobilization. However, IMNs may not suit everyone and can carry risks of infection or complications, highlighting the need for careful consideration.
Cost is another factor in the discussion. While the initial costs of IMNs are higher, the potential reduction in rehabilitation expenses can make them more economical overall. A health economics study suggested that faster recovery may offset the upfront investment in flexible nails, yet not all clinics can provide this technology. Ultimately, the choice between IMNs and traditional casting requires a nuanced understanding of individual patient needs and circumstances.
Why Choose Flexible Intramedullary Nails for Bone Fractures?
| Parameter | Flexible Intramedullary Nails | Traditional Casting Methods |
|---|---|---|
| Weight | Lightweight | Relatively Heavy |
| Mobility | High (Allows partial weight-bearing) | Low (Immobilizes the limb) |
| Infection Risk | Low (Invasive but controlled) | Variable (Potential for skin breakdown) |
| Healing Time | Faster (Stabilizes fracture immediately) | Slower (Dependent on cast duration) |
| Flexibility | Excellent (Accommodates variable anatomy) | Limited (Rigid support) |
| Usability | Less time-consuming | Time-consuming (Application & removal) |
Biomechanics of Flexible Intramedullary Nails in Fracture Healing
The biomechanics of flexible intramedullary nails play a crucial role in fracture healing. These devices are designed to accommodate the natural movements of the bone during the healing process. Research indicates that flexible nails provide micromotion at the fracture site, which is essential for bone regeneration. A study reported that 85% of patients with long bone fractures using flexible nails achieved union without complications. This success rate suggests that the biomechanics of these nails facilitate a favorable environment for healing.
Moreover, flexible intramedullary nails reduce stress concentration. Traditional rigid fixation can lead to non-union or delayed healing in certain fractures. The flexible nature allows the nails to bend with the bone's physiological movements. Interestingly, a biomechanical analysis revealed that these nails can withstand loads of up to 300 Newtons before yielding. However, not every case results in optimal healing. There can be variability in patient outcomes, influenced by factors like age or bone quality.
It's important to acknowledge that the use of flexible intramedullary nails is not without its challenges. Despite high success rates, some patients may experience discomfort or complications. This highlights the need for ongoing research into the materials and designs of these nails. Adjustments and refinements can further enhance their effectiveness and reliability in clinical practice.
Indications and Contraindications for Using Flexible Intramedullary Nails
Flexible intramedullary nails (IM nails) are often chosen for treating bone fractures, particularly in pediatric patients. They are suitable for fractures of long bones, like the femur and tibia. However, certain conditions may limit their use.
Fractures in patients with significant bone loss might not heal well with flexible IM nails. Similarly, complex fractures or those with delayed healing can pose challenges in treatment. Infections in the area of the fracture also contraindicate the use of these nails.
**Tip:** Always assess the fracture type and location before choosing a treatment method. Effective diagnosis can enhance recovery outcomes.
Bone stability is key when considering flexible IM nails. Patients with multiple fractures may require a different approach. An inadequate understanding of the patient’s overall condition can lead to poor decisions.
**Tip:** Consult with a specialist when in doubt. A second opinion can often provide clearer insights into the best approach.
The choice of using flexible intramedullary nails should balance benefits with potential drawbacks. Always remember that individual patient needs vary greatly.
Post-Surgical Care and Rehabilitation with Flexible Nails
Post-surgical care and rehabilitation are crucial for patients who receive flexible intramedullary nails for bone fractures. Studies show that proper rehabilitation can improve recovery outcomes significantly. Up to 85% of patients report reduced pain and better mobility within weeks after surgery. Early weight-bearing activities support bone healing. However, some patients struggle with adhering to rehabilitation protocols. This can delay progress and negatively impact long-term results.
Physical therapy often begins shortly after surgery. Patients are encouraged to perform gentle range-of-motion exercises. A report indicated that patients who engage in early physical therapy see a 30% faster recovery than those who delay it. Consistent follow-up appointments are essential to monitor healing. Still, some issues may arise, such as excessive swelling or discomfort. These may require adjustments to the rehabilitation plan, which can be frustrating for patients.
Understanding the mental aspect of recovery is also important. Many patients feel anxious about their progress. This anxiety can hinder their willingness to participate in rehabilitation activities. Creating a supportive environment, involving family or peers, can empower patients. Encouraging open communication about struggles fosters a collaborative mindset between patients and healthcare providers.